
The International Society for Blood Transfusion now officially recognises the SARA antigen as a new blood group, and, for the young SARA-positive males in the families, this discovery means that they and their families will be able to successfully manage future pregnancies where the SARA antigen may be inherited. The Blood (Type) of Jesus: AB Please be aware that throughout the centuries there are and have been plenty of scientists and religious prominence openly expressing their views that the Shroud of Turin is a fake. When the final analysis was complete, they discovered that in SARA-positive individuals a single nucleotide had changed in the DNA sequence which encodes glycophorin A, one of the main proteins on the surface of the red blood cell. The analysis found nearly 500,000 single nucleotide variations in the Australian family, so finding the one variation responsible for the SARA antigen was an incredibly detailed and painstaking task.ĭespite the laborious nature of the task, Rhiannon systematically refined the data. “Because SARA is so rare, we knew we were looking for something that hadn’t been discovered before (and) we also had to look for something which fit the inheritance pattern.” It’s a leading-edge technology that wasn’t widely available to the research world even five years ago,” said Rhiannon. The majority of people, about 85, are Rh-positive. If you don’t have the protein, you’re Rh-negative. If you have the protein, you’re Rh-positive. You inherit the protein, which means you get your Rh factor from your biological parents. “We used whole exome sequencing, which reads the entire coding region of a person’s DNA. Rh factor (or Rhesus factor) is a type of protein on the outside or surface of your red blood cells. The next step was to find a gene sequence shared only by those family members. To identify the gene, researchers first identified the family members who carried the antigen by checking whose blood reacted with the antibody in the Canadian mother’s plasma. Blood and DNA samples were taken from both the Canadian and Australian families, including members from several generations of each family. With the problem identified as SARA incompatibility, a Lifeblood research team, led by Professor Catherine Hyland, set out to identify the gene responsible. The baby needed a double volume exchange transfusion to recover.” She had an antibody that reacted strongly with SARA-positive cells. Rhiannon McBean, a doctoral candidate in Research and Development at Lifeblood and the University of Sydney, explained the results. “The father was SARA-positive and the mother was SARA-negative. The mother’s plasma was tested against a panel of over 50 archived rare cell types, and reacted only with a sample of SARA red cells. 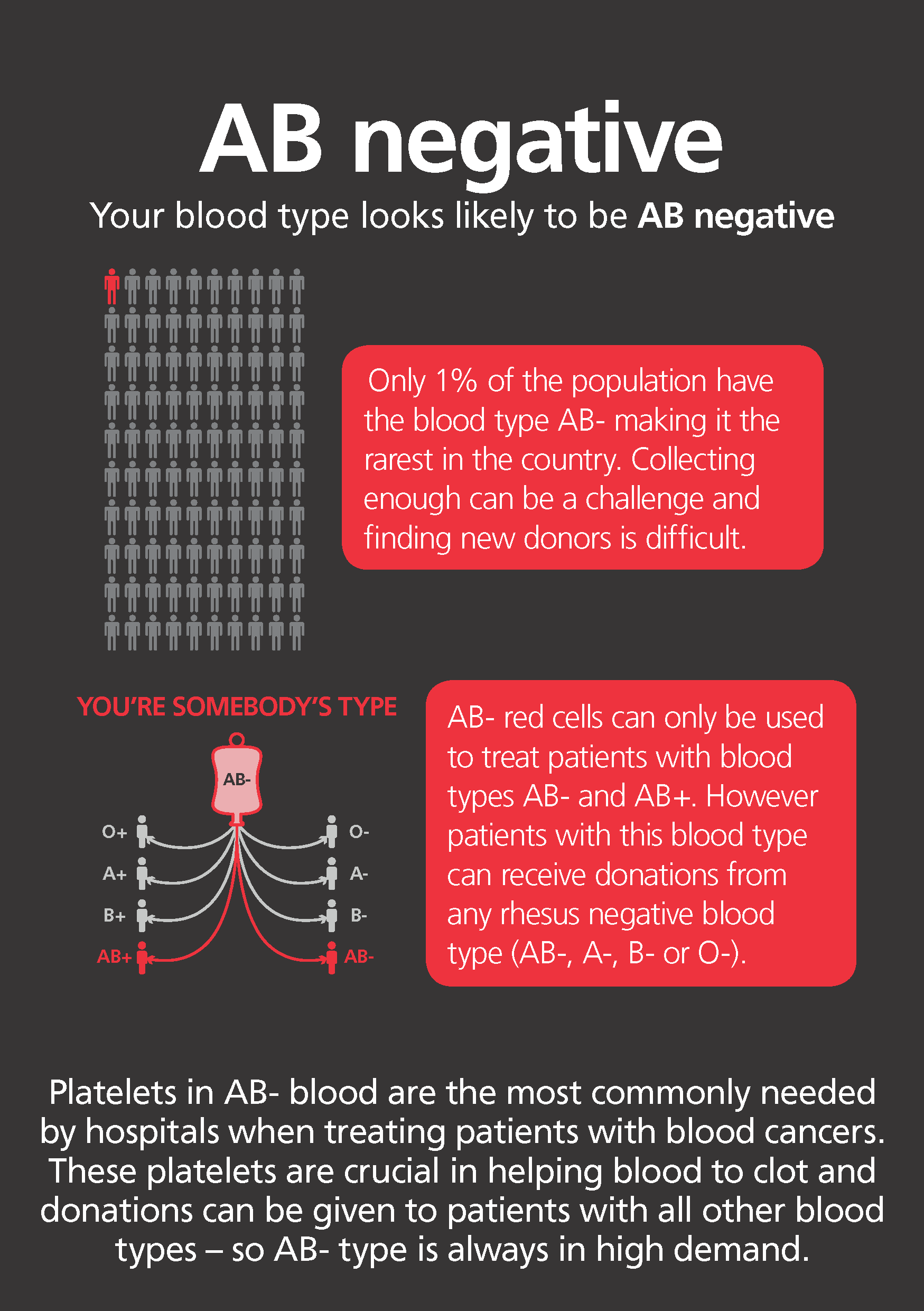
The Canadians thought that this case could be related to the rare SARA antigen and sent samples to Australia for confirmation. SARA didn’t fit into any of the known families of blood group antigens, so a vial of Sarah’s unusual blood was frozen and stored in a blood type archive.Īround 20 years later, Lifeblood received blood samples from collaborators at the Canadian Blood Service which came from a family whose baby had needed a massive blood transfusion at birth. The new antigen was named after her: ‘SARA’. In 1990, researchers at the National Blood Group Reference Laboratory found a novel antigen on the red cells of a single, very dedicated blood donor named Sarah. Modern genetic techniques allow rare blood variants to be characterised with pinpoint accuracy, and researchers at Lifeblood have used them to solve the medical mystery of a Canadian baby who nearly died at birth. There are hundreds of possible variations apart from the commonly known ABO and Rhesus blood groups. 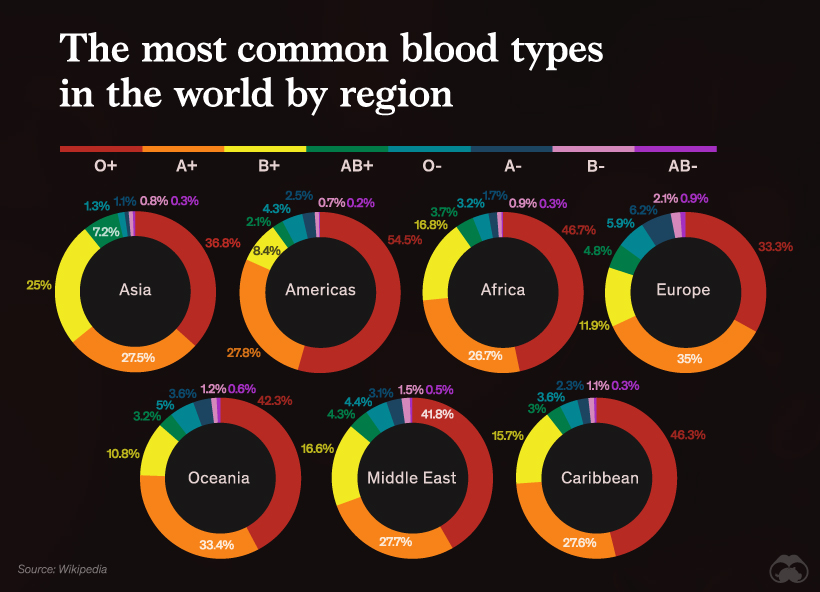 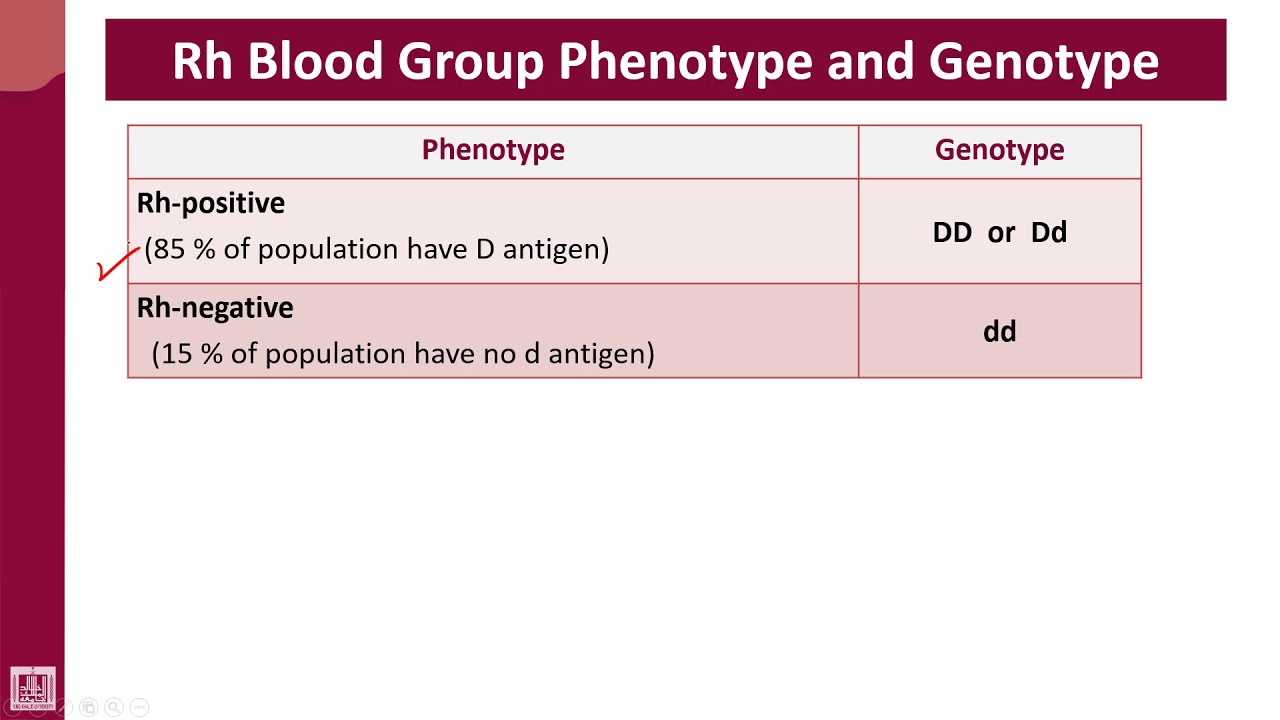
The eight most common blood types are a result of the different combinations of A, B, O and the Rh factor - A+, A-, B+, B-, O+, O-, AB+, AB-.Your blood type is more complicated than you think. There is also a protein called the Rh factor which, if present, makes your blood positive (+) and if not, your blood type is negative (-). Visit our blood types blog if you want to read more. When both are present, that is called blood type AB, and when neither are present, it’s called blood type O. Same is true for the B antigen and blood type B. When only the A antigen is present, you are blood type A. Two antigens on your red blood cells determine type: A and B. Thankfully, in the many centuries since blood transfusions were first attempted, doctors and researchers discovered our different blood types and determined each type’s compatibility with other types. Otherwise, the transfusion may do more harm than good. When a patients need a blood transfusion, it’s important they receive a blood type compatible with their own.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
